
Anyone can get chronic kidney disease (CKD) at any age.
Some people are more likely than others to develop kidney disease, including those with:
- Diabetes
- High Blood Pressure
- A Family History of Kidney Disease
Also, people who belong to a population group with a high rate of diabetes or high blood pressure, such as African Americans, Hispanic Americans, Asian, Pacific Islanders, and American Indians are more vulnerable to developing chronic kidney disease.
For people with diabetes, the deterioration that characterizes kidney disease takes place in and around the glomerule, the blood-filtering units of the kidneys. Early in the disease, the filtering efficiency diminishes, and important proteins in the blood are lost to the urine. Medical professionals gauge the presence and extent of early kidney disease by measuring protein in the urine. Later in the disease the kidneys lose their ability to remove waste products, such as creatinine and urea, from the blood.
Symptoms related to End Stage Renal Disease (ESRD) or kidney failure usually occur only in the late stages of CKD, when kidney function has diminished to less than 25% of normal capacity. For many years before that point kidney disease of diabetes exists as a silent process.
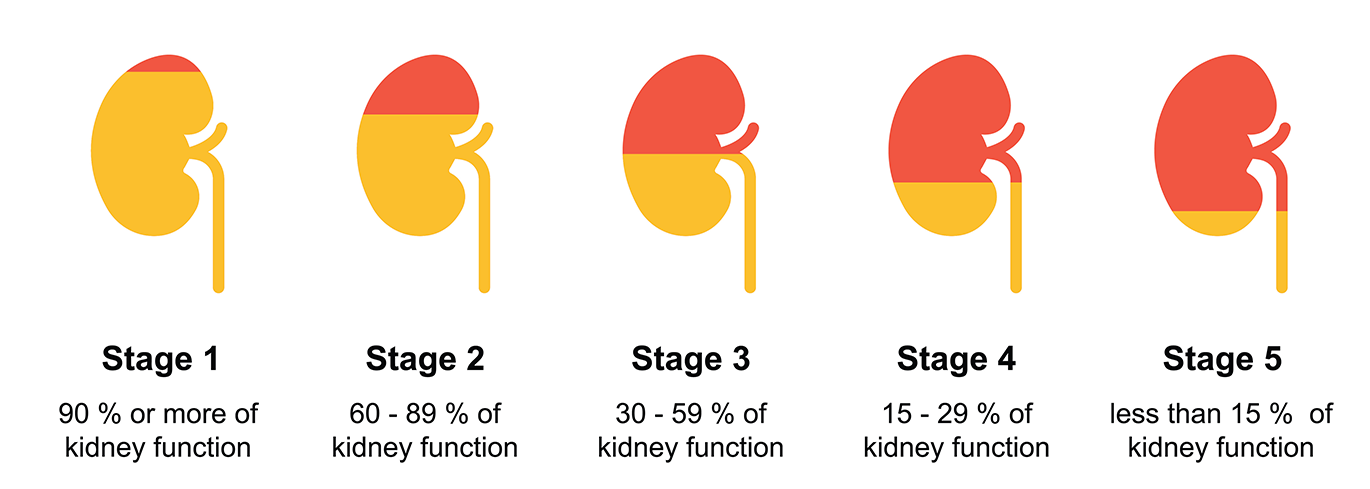
ESRD PROGRESSION
Stage I
The flow of blood through the kidneys, and therefore through the glomeruli, increases – this is called hyperfiltration – and the kidneys are larger than normal. Some people remain in stage I indefinitely; others advance to stage II after many years.
Stage II
The rate of filtration remains elevated or at near normal levels, and the glomeruli begin to show damage. Small amounts of a blood protein known as albumin leak into the urine – a condition known as microalbuminuria. In its earliest stages, microalbuminuria may come and go. But as the rate of albumin loss increases from 20 to 200 micrograms per minute, microalbuminuria becomes more constant. (Normal losses of albumin are less than 5 micrograms per minute.) A special tests is required to detect microalbuminuria. People with NIDDM and IDDM may remain in stage II for many years, especially if they have normal blood pressure and good control of their blood sugar levels.
Stage III
The loss of albumin and other proteins in the urine exceeds 200 micrograms per minute. It now can be detected during routine urine tests. Because such tests often involve dipping indicator strips into the urine, they are referred to as “dipstick methods.” Stage III sometimes is referred to as “dipstick-positive proteinuria” (or “clinical albuminuria” or “overt diabetic nephropathy”). Some patients develop high blood pressure. The glomeruli suffer increased damage. The kidneys progressively lose the ability to filter waste, and blood levels of creatinine and urea nitrogen rise. People with IDDM and NIDDM may remain at stage II for many years.
Stage IV
This is referred to as “advanced clinical nephropathy.” The glomerular filtration rate decreases to less than 75 milliliters per minute, large, amounts of protein pass into the urine, and high blood pressure almost always occurs. Levels of creatinine and urea-nitrogen in the blood rise further.
Stage V
The final stage is ESRD. The glomerular filtration rate drops to less than 10 milliliters per minute. Symptoms of kidney failure occur.These stages describe the progression of kidney disease for most people with IDDM who develop ESRD. For people with IDDM, the average length of time required to progress from onset of kidney disease to stage IV is 17 years. The average length of time to progress to ESRD is 23 years. Progression to ESRD may occur more rapidly (5-10 years) in people with untreated high blood pressure. If Proteinuria does not develop within 25 years, the risk of developing advanced kidney disease begins to decrease. Advancement to stages IV and V occurs less frequently in people with NIDDM than in people with IDDM. Nevertheless, about 60 percent of people with diabetes who develop ESRD have NIDDM.

